Foot and ankle injuries are among the most common musculoskeletal claims in California’s workers’ compensation system. From repetitive stress disorders to acute trauma, these cases often raise disputes about causation, apportionment, and long-term impairment. A qualified medical examiner in California plays a critical role in clarifying these medical questions.
This article explains how foot and ankle injuries workers compensation cases are evaluated, how a podiatric QME evaluation supports fair compensation decisions, and why structured reporting is essential in resolving disputes.
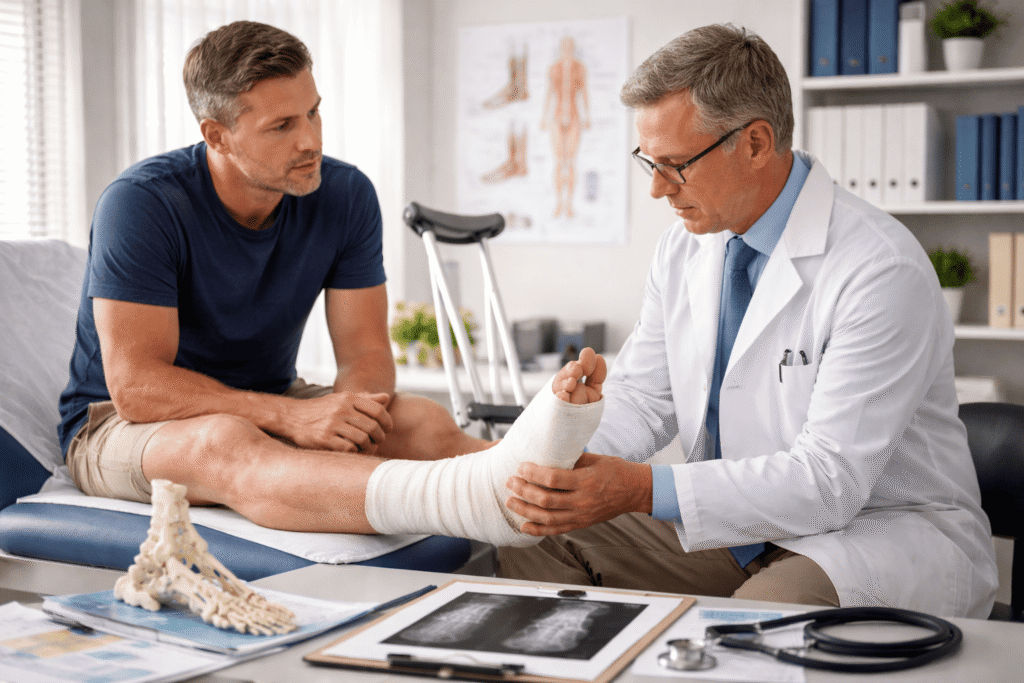
Common Foot and Ankle Claims in Workers’ Compensation
Foot-related claims frequently arise in physically demanding occupations. Construction workers, warehouse employees, healthcare staff, and service industry workers often present with conditions such as:
- Ankle sprain workers comp claim
- Plantar fasciitis workers compensation
- Achilles tendon injury workers comp
- Foot fracture workers compensation case
In ankle injury workers compensation California disputes, employers or insurers may question whether the condition is truly work-related or partially attributable to pre-existing degenerative factors.
Similarly, cumulative trauma cases involving prolonged standing or repetitive movement may evolve into complex podiatry workers compensation cases. Determining whether symptoms stem from occupational exposure or unrelated pathology requires a structured medical-legal analysis.
A thorough evaluation of work-related foot injuries provides clarity not only for the injured worker but also for legal stakeholders assessing benefit eligibility.
The Role of the Podiatric QME Evaluation
A structured podiatric QME evaluation serves as an independent medical-legal assessment designed to resolve disputes in a foot injury workers comp claim. The QME does not provide treatment; instead, the physician performs an objective analysis of causation, extent of injury, impairment rating, and need for future care.
Under the oversight of the California Division of Workers’ Compensation Medical Unit<, QMEs must adhere to reporting and evidentiary standards. The podiatric specialist reviews medical records, diagnostic imaging, treatment history, and occupational demands before issuing conclusions.
This process is essential when compensation hinges on medical findings. Whether assessing a ligament tear or chronic heel pain, the evaluator’s analysis determines whether disability benefits, permanent impairment ratings, or apportionment apply.
Physicians who understand structured documentation principles often strengthen defensibility, particularly in alignment with reporting guidance.
How QME Findings Influence Compensation Decisions
In disputed ankle sprain workers comp claim or Achilles tendon injury workers comp cases, medical opinions directly influence financial outcomes. A QME’s report may determine:
- Whether the injury arose out of employment
- The percentage of permanent impairment
- The degree of apportionment to pre-existing conditions
- The necessity of future surgical intervention
For example, in a foot fracture workers compensation case, the evaluator must determine if delayed healing resulted from work conditions or unrelated comorbidities.
In chronic conditions such as plantar fasciitis workers compensation, disputes often involve whether prolonged standing at work materially aggravated the condition.
Accurate medical reasoning protects both parties. When well-supported, a podiatric medical-legal opinion reduces litigation exposure and expedites resolution.
For broader insight into compensation impact, see Understanding the Impact of Permanent Disability Ratings on Your Workers’ Compensation Benefits.
The Step-by-Step QME Process in Foot Injury Cases
The process typically begins when a dispute arises regarding causation or impairment. After panel selection or agreement, the qualified medical examiner in California schedules the evaluation.
The QME then:
- Reviews complete medical records
- Conducts a physical examination
- Assesses occupational duties
- Determines impairment under AMA Guidelines
- Issues a formal report
This podiatric medical legal evaluation California must follow regulatory structure and evidentiary standards outlined in workers’ compensation law (general overview of workers’ compensation process: Workers’ Compensation System Overview.
When procedural clarity is maintained, disputes often resolve without prolonged litigation.
Why Podiatric Expertise Matters in Workers’ Comp
Foot and ankle pathology often involves complex biomechanical analysis. Differentiating between degenerative tendon changes and acute occupational injury requires specialized expertise.
A podiatric QME can assess gait abnormalities, functional limitations, and long-term prognosis more precisely than a general evaluator. In cases involving surgical outcomes, residual instability, or nerve involvement, specialty analysis strengthens the credibility of the final report.
Professional communication and clarity also influence how reports are received by attorneys and judges.
Operational Considerations for QME Practice
High-volume foot and ankle evaluations require structured workflow and administrative coordination. Many physicians rely on a specialized QME management company to handle scheduling, billing, and documentation logistics.
Efficient operations allow podiatric specialists to focus on clinical analysis rather than administrative burden. Financial structure and revenue considerations are discussed in.
Physicians evaluating whether to operate independently or partner with support infrastructure may also explore this post.
For injured workers and referring professionals seeking specialized evaluators, you can also check our QME doctors.
Conclusion
Foot and ankle claims are medically nuanced and financially significant within California’s workers’ compensation system. A structured podiatric QME evaluation provides objective analysis that supports fair compensation, clarifies causation disputes, and strengthens case resolution.
From acute trauma to chronic cumulative injury, the role of the QME is central to ensuring evidence-based outcomes. Accurate medical reasoning, regulatory compliance, and clear documentation ultimately determine whether compensation decisions are timely and defensible.
